Quick Summary
Your hospital workflow breaks when departments do not share information well. Patients wait longer. Staff get frustrated. Follow-ups get missed. This post shows where handoffs fail and how to build smoother connections from the front desk to post-discharge care without overhauling your entire system.
Table Of Contents
Introduction
When a patient walks into your hospital, the real work begins. But what happens after they check in? Most facilities handle each step separately. The front desk does its job, the nursing staff does theirs. The billing team works in the background, yet when you watch the full picture from start to finish, you can see many challenges. This gap creates repeated delays, lost information, and frustrated patients who feel forgotten once they leave. The problem is the broken handoffs between departments. In this blog post, we will show you exactly where these gaps hide and how fixing them transforms your entire healthcare operations into one smooth journey.
Key Takeaways
Information gets lost between departments.
Handoffs fail at admission, stay, discharge, and follow-up.
Connected software cuts missed follow-ups.
Real-time views help clear delays faster.
You can connect old systems without replacing them.
The Main Challenge Why Traditional ERP Falls Short
When different departments are not well connected, there can be serious effects across the hospital. If the emergency department cannot find an empty bed, it slows down new patients coming in by ambulance. The scheduled surgeries get pushed back, and the staff feels the stress. This is not just an emergency room issue and shows a failure in clinical process management. Small delays in one place create bigger problems everywhere else.
How One Slow Step Affects Everything
The problems can also be seen in many daily tasks that happen manually and remain disconnected. Referral letters get misplaced, and the insurance checks take too long. Discharge summaries do not reach family doctors on time. This extra work adds up quietly. It is a major but often ignored part of healthcare operations management.
How Workflow Gaps Affect Revenue and Patient Safety
These breakdowns directly affect results that matter, and patients need to stay longer than needed. Mistakes become more likely. Your team feels tired and overworked. Patients notice and leave unhappy. Fixing your hospital workflow is not just about being organized. It protects your patients and your finances at the same time.
Know more about Hospital Management Software.
A Step-by-Step Breakdown of Where Workflows Break
Let us understand where workflows break down in a hospital. These are the handoff points where things get delayed or lost.
The Access & Admission
When registration is slow or insurance details are wrong, the patient’s visit starts badly. Triage gets backed up. People wait longer than needed. The right hospital workflow software can fix these early delays by checking details automatically and moving patients forward faster.
The Inpatient Stay: Capacity & Care Coordination
Inside the hospital, things slow down when departments do not share information well. A doctor waits for a lab result. A patient waits for a consult. Beds stay empty while new patients wait in the ER. This part of clinical operations needs better communication and real-time bed tracking to keep moving.
Choose the best Healthcare ERP.
The Discharge Planning
Getting a patient ready to leave is the hardest handoff. Planning often starts too late. Staff cannot arrange transport or post-care beds in time. Small things like a pending therapy session cause long delays. These problems need attention early, not at the last minute.
The Follow-Up: Post-Discharge & Referrals
After the patient goes home, work remains. Referral letters get lost. Follow-up calls are missed. Patients do not show up for their next appointment. This is a weak spot in the patient journey. When follow-up fails, readmissions go up, and recovery takes longer.
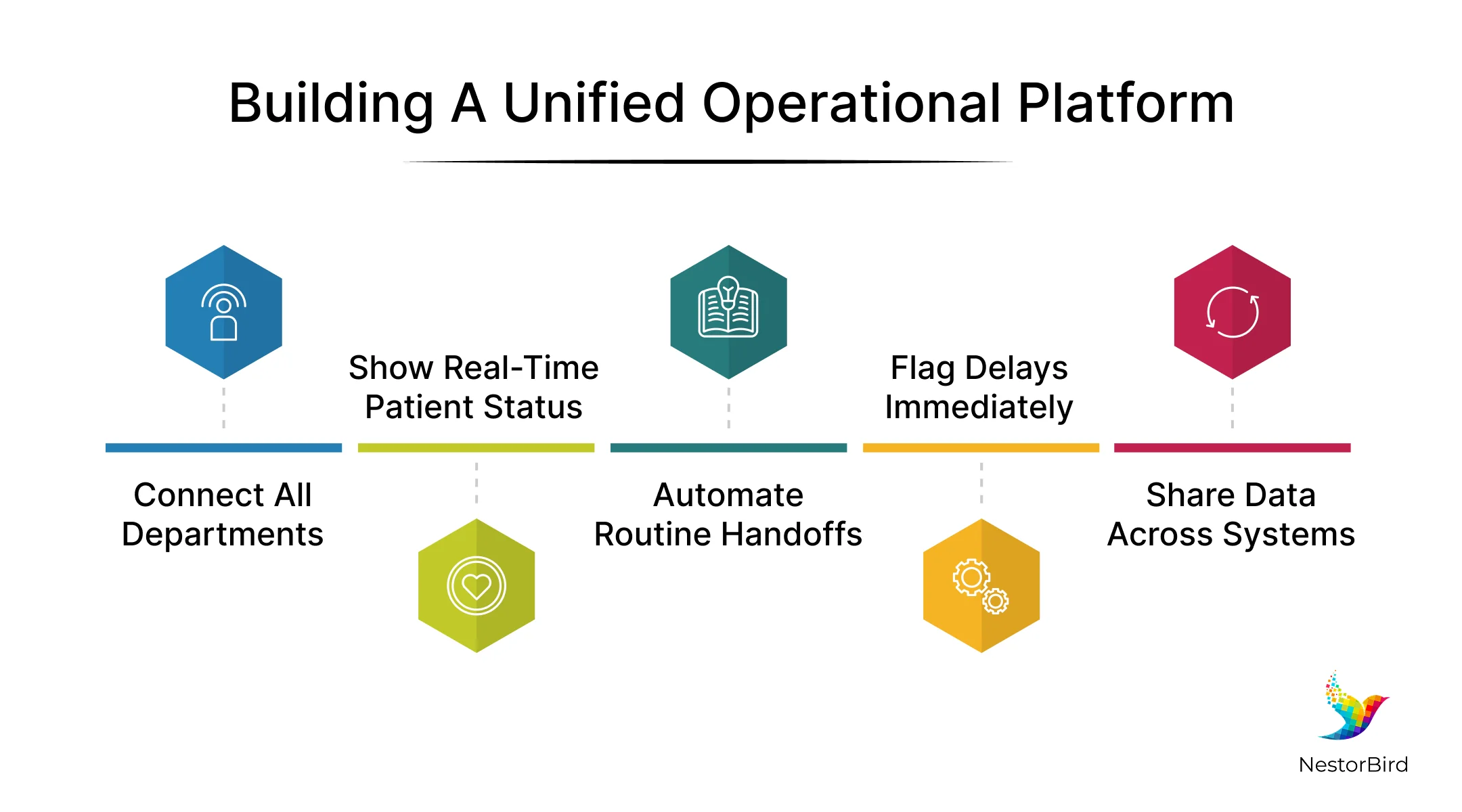
Building and Implementing a Unified Operational Platform
When you have an efficient unified system that connects all departments, things start running more smoothly. The goal is to move from separate workflows to one connected platform.
The Solution: A Central View of Operations
Some hospitals now use a central team to watch patient flow across the entire facility. This gives them real-time updates on where delays are happening. They can see bed availability, discharge progress, and pending tasks in one place. This approach improves hospital workflow management by giving everyone the same picture at the same time.
The Role of Technology
Modern tools help predict problems before they happen in hospital workflow processes. An automated workflow hospital setup can flag which patients might face discharge delays. It can suggest the best bed for each new patient. It handles repetitive jobs like uploading documents or entering referral data, which frees up your staff for more important work.
This is why healthcare organizations need an ERP.
Integration over Replacement
Most hospitals already have systems they use every day, and the better path is using hospital workflow software that connects your existing tools. It pulls information together in one place. This creates a single source of truth without forcing your team to learn everything from scratch.
Check out the benefits of ERP in the healthcare industry.
Conclusion
When no single team in hospital operations owns the full patient journey, small delays keep adding up. The front desk may be working efficiently, yet important information gets lost when moving from one department to the next. Fixing this can be achieved by having a unified system in place for your hospital. If you are ready to build this connected system, solutions from NestorBird help you link every step from check-in to follow-up. Theplatform gives your team one clear view of the entire workflow, so nothing gets lost between departments.
Frequently Asked Questions
Start by mapping every step from check-in to follow-up. See where delays happen most. Then add software that connects those steps automatically. You do not need to change everything at once.
Use a simple structure like I-PASS during every handoff. This means sharing illness severity, patient summary, action lists, and allowing the receiver to ask questions. Face-to-face handoffs work best.
Different departments use separate systems that do not talk to each other. A referral entered in one place never reaches the next team. Connected software solves this by showing the same data everywhere.